Warning-this article contains graphic photos of staph infections

Definitions
- Commensal-when one organism obtains food or other benefits from another organism without harming or benefiting the other organism.
- Exotoxin-toxins released from bacteria that can cause damage and harm.
- Folliculitis-an infection of a hair follicle.
- Microbiota-the group organisms that form ecological communities that live within us and on our skin. They include bacteria, viruses, fungi, and other microorganisms. They can be beneficial, neutral, or pathogenic.
- MRSA (Methicillin-resistant staphylococcus aureus)-an antibiotic-resistant form of staph.
- Opportunistic pathogen-a pathogen that takes advantage of an altered environment, such as a disturbance in the immune system.
- Pathogen-a disease-causing organism. These include bacteria, viruses, fungi, protozoa, and worms.
- Sepsis-an infection that enters the bloodstream where the body’s response causes potential damage to organs and tissues. This is an emergency medical condition.
- Slough (‘sluff’)-a mass of dead cells and tissue seen during the inflammatory phase of wound healing.
- Toxic shock syndrome-a life-threatening disorder caused by the release of toxins from bacteria. In the 1970s, it caused a number of cases through the use of super-absorbent tampons.
Background
Staphylococcus aureus (‘staph’) is a gram-positive bacteria commonly found on human skin and in the upper respiratory tract. While it is generally a commensal component of the skin microbiota, it can also become an opportunistic pathogen leading to skin infections, sinusitis, and food poisoning. It can also lead to lethal conditions such as toxic shock syndrome and bacterial sepsis. In this article, I will be focusing on treating its place in skin infections.
Some of the common skin infections I see in first aid are open infections, abscesses, folliculitis, and boils.
Staph exhibits extensive genetic variation, though only a limited number of these variants pose a risk for human health. While there are multiple strains of staph, they are often clinically divided by those that are resistant to antibiotics and those that are not. The most common pathogenic strain is Methicillin-resistant staphylococcus aureus (MRSA), which can be hospital-acquired or community-acquired (meaning that it is spread in a non-healthcare setting). It is one of the most common hospital-acquired infections in the US, with up to 500,000 cases a year.
There is currently no vaccine for Staphylococcus aureus.
Contagiousness and Patient Education
Staph is contagious through multiple pathways, including skin-to-skin contact, pus, and fomites such as towels and clothing. This means health care workers must be cautious to avoid spreading this infection while administering treatment as well as disposing of infected materials.
It is important to discuss possible contiguousness with patients. This is especially true for some of the events where hugging is commonplace, as well as people volunteering in kitchens and other places where there is potential for spreading the infection.
In these situations, It is useful to discuss what staph is and what it is not, and that it is a common infection. This helps people not feel bad or guilty about having this condition, which limits their capacity to touch others or work in places where it could spread. If they felt guilty, they may want to hide that they have staph and are more likely to spread it.

Personal Interest and Experience
I have been working at wilderness first aid clinics for over 25 years. Staph infections are common in these settings and range from mild to severe (though not toxic) forms. The infections are due primarily to the lack of available hygiene and sanitation. Also, since cuts and scratches are common in these rougher environments, there is more opportunity for infection to occur. Lowered immune resistance may be another factor.
The medical professionals on staff have taught me a lot, increasing my skill level in both diagnosis and treatment. I’ve learned how to lance abscesses and have gained more knowledge on which antibiotics may be the most appropriate and when hospitalization may be necessary.
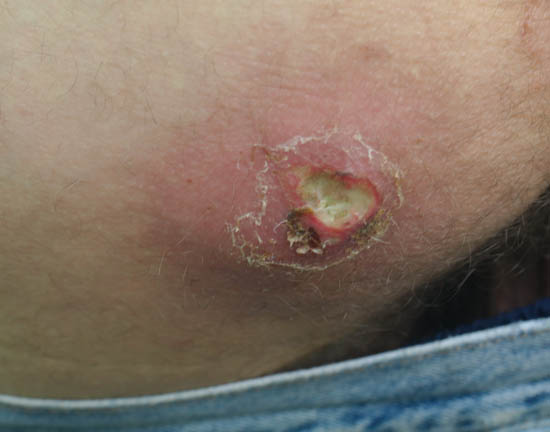
Assessment and Diagnosis
Assessment and diagnosis is based on visual and physical examination. Since Staphylococcus aureus is the most common bacteria to cause skin infections, it is usually assumed to be the causative agent when seeing a skin infection. We cannot culture the infection at these events, so we have no definitive way of knowing whether it is MRSA or not. And as MRSA and non-MRSA infections present similarly, we tend to treat them similarly, with the severity of the infection determining the course of action.
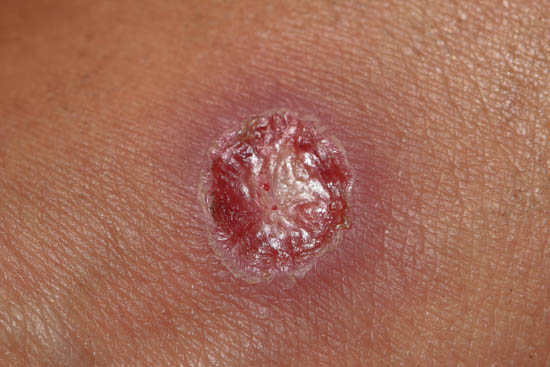
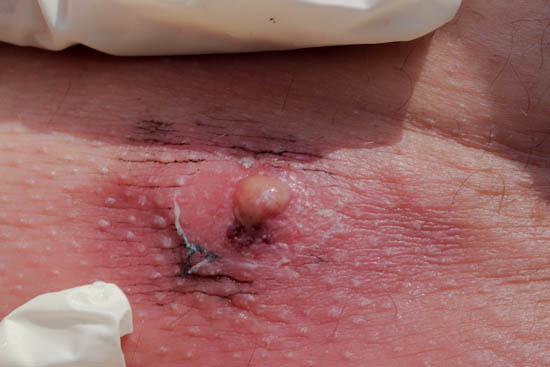
Spider bite or Staph Infection
It is common for people to think they have a spider bite when they have a staph infection. There are a couple of reasons for this, including that both often show up with no warning and can have a similar appearance. Since the bite of a spider is usually not felt, this can seem like a reasonable conclusion. Still, the reality of my experience is that the majority of people who think they have spider bites have staph infections. This is echoed by other medical sources. It seems people would rather have a spider bite, which is somehow ‘cooler’ (and non-contagious) than a staph infection.
Spider bites range from non-harmful (the majority) to venomous, and those can cause a lot of tissue damage. They can also become infected, so that adds another layer of complexity with diagnosis and treatment.
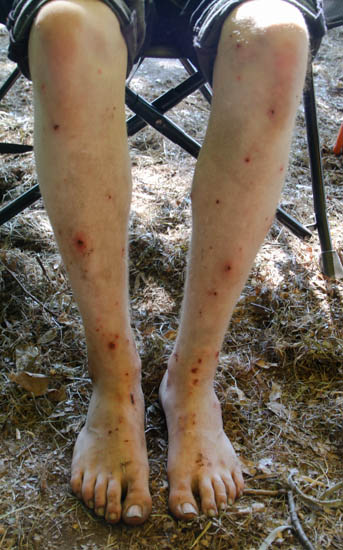
Importance of Sanitation
Due to the contagiousness of Staphylococcus aureus, it is pertinent to make sure all infectious waste is kept in a safe place where a human, dog, or other animals will not get into it. It does not need to go into hazardous waste, just to be kept safe. The waste products include dirty gauze pads and similar equipment as well as the wastewater. And since the bacteria can last for up to 24 hours and longer on surfaces and fabric, people should know that their clothes and bedding might harbor staph bacteria. Health care workers should wear gloves and dispose of them properly and wash well afterward, including sterilizing any tools involved.
Treatment Protocols
Treatment Protocols
There are a few main strategies that I use for staph infections, which have changed over time. Internally I use a variety of herbs to help bolster immunity and fight infection. Externally I use both herbs and activated charcoal topically as well as medicinal soaks.
Treatment
Step 1-Options
Once a diagnosis is established, the first question for treatment is whether to use herbs, antibiotics, or both. This is primarily up to the patient. The options and considerations are discussed for both antibiotics and herbal medicines with each individual. Our goal is to provide agency for the patient, so they have the information to make informed personal choices.
If the patient wants antibiotics, a new set of choices emerges. Sometimes we have the antibiotics and the staff to administer them, but oftentimes we do not. If we don’t, they will have to go to a clinic or hospital, which will take time and money. So this partially depends on the individual’s resources. Also, many folks have had bad medical experiences making them resistant to seek medical help even if we think it is a good idea.
When discussing the options, we let the person know that taking herbal remedies will likely take longer and can be more complicated than pharmaceuticals. By ‘difficult’, I mean that they will generally have to come in at least once a day to have their bandages changed, wounds washed, and to have the remedies re-applied. They may also need to take the herbal preparations orally 2-3 times daily. The advantage is that we have the medicine at the first aid station, so they are available and free. And some people would rather use plant-based medicines than pharmaceuticals.
If the staph appears to be spreading, or if there is lymphangitis (red lines caused by the bacteria entering the lymphatic vessels), we set up a timeline, and if we don’t see improvement within a specific time frame, we suggest getting antibiotics. The timeframe is based on two main factors. The first is the virulence of the infection and how fast it is spreading. The other consideration is the patients’ own decision of how long they feel comfortable waiting until seeking further help. Again, we talk each person through these choices and try to give applicable and transparent information.
There are definitely times we suggest they seek immediate medical help. This is often due to the severity of the infection, especially if it is spreading rapidly or it is on their face where it might leave a scar. The other time we suggest medical assistance is when the person seems resistant to our helping them, and may spread the infection. If someone chooses the pharmaceutical route, we will give them whatever information we have about the closest clinics around. Depending on where the even it held, they could be a few hours away.

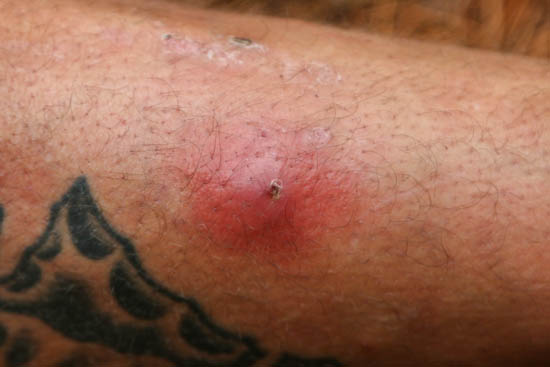
Opening and Draining Abscesses
Abscesses are a type of infection where the pus accumulates beneath the skin. They are often caused by staph bacteria and generally need to be opened and drained. Afterward, herbal remedies can be applied externally. Hot/warm compresses can be applied to an abscess close to opening to help it open fully and drain. Sometimes it is necessary to lance the abscess to allow it to drain. Anyone doing this should know the proper technique as well as have the proper tools. Sterilized scalpels or needles are used to open the abscess. For learning how to drain an abscess, I suggest working with an experienced professional. It is helpful to give pain-relieving and sedative herbal preparations beforehand, such as Hops and Valerian. If there is a medical person on staff, they can administer lidocaine before lancing to help relieve pain.
After it is opened, it can be useful to pack the open abscess with iodoform-packing strips. This is a thin roll of gauze permeated with a form of iodine to help it drain and prevent infection. These strips are packed into the now opened abscess with the wooden end of a cotton tip applicator or other tools. A short wick is left outside the hole. Each day some of the strip is pulled out and cut off. This helps the abscess drain and heal properly.
Abscesses can also be soaked in a strong herbal tea to help soften them as well as for their disinfectant properties. Herbs that are useful for this include Chaparral, Yarrow, and plants in the genus Berberis such as Oregongrape root and Barberry. Make sure the basin is clean before and after each use by either using a plastic liner or disinfecting it with bleach or another antiseptic cleanser.
External Applications
I generally alternate between herbal preparations (liniments and tinctures) and activated charcoal. I usually begin with the former, as they are easier to prepare and clean up. If after applying the herbal preparations and the infection seems to be clearing up quickly, I may stick to this treatment protocol. If the infection continues to worsen or does not appear to get better, I alternate between the two. The main way of knowing that an infection is worsening is that instead of engaging the healing process, the wound festers, potentially getting deeper, and is often filled with pus.
These treatments are usually applied daily for each staph infection on a person’s body. This can take a long time depending on how many staph infections they have, as there can be many per individual. After the initial examination, it is helpful to let them know approximately how long it may take to do this daily. This can help them make a decision. They may choose to seek conventional medical care, as the process is more straightforward and potentially less time-consuming, at least on a daily basis, though likely more expensive and initially more time-consuming as they will have to go to a hospital or clinic.
External Applications-Activated Charcoal
Activated charcoal can be used externally to adsorb bacteria and exotoxins from the skin surface. There are two ways to apply the activated charcoal poultice. It can be placed on a piece of gauze and the activated charcoal side can be applied directly on the infection, or the activated can be made into a ‘sandwich’ in which is held between two pieces of gauze, and the gauze is placed over the wound.
It is important to use absorbent gauze with the activated charcoal sandwich so that it can wick up bacteria and exotoxins. Note the differences between absorb and adsorb. An absorbent assimilates the material throughout its body as with a sponge or gauze pad. In adsorption, the substance binds to the surface of the adsorbent material, such as the silica packets packaged with foods to adsorb moisture. Adsorption is an essential property of activated charcoal as it creates a tighter bond with the substance (bacteria or toxin), more effectively eliminating it from the infection site.
When the infection is not as deep or severe, the activated charcoal can be applied directly to the surface of the infection. When the infection cavity is deep, the activated charcoal sandwich is useful as it avoids depositing the charcoal directly into the wound, making it more difficult to clean up and heal.
To prepare the poultice, first moisten the activated charcoal in a container until it is slightly muddy in texture. Then spread it about 1 mm or so thick on a gauze pad. When making an activated charcoal sandwich, another gauze pad is placed on top of the activated charcoal, so it is held between two absorbent gauze pads. In both cases the poultice must be in direct contact with the infection. It should be held snugly but not too tightly against the infection.
Activated charcoal can be messy, and occasionally, after the gauze is removed, the patient feels a moment of distress as they see that the wound area is now black. They should be informed that this is just the activated charcoal and will eventually wear off. Gently wash off the charcoal between applications.

External Applications-Herbal Preparations
There are a number of herbal tinctures and liniments that can be applied on gauze pads and applied topically to help with staph infections. While both tinctures (based in ethanol) and liniments (based in isopropyl alcohol) are effective, I prefer liniments as they are less expensive to prepare, and most first aid work is done for free. The advantage of tinctures is that they can also be taken internally.
Apply the below plant extracts directly onto a gauze pad until it is moist but not overly saturated.
The individual plants used in the tinctures and liniments come from several categories. I tend to use two antibacterial, one antiinflammatory, and one astringent herb. I keep these as individual medicines and mix them up as needed as well as having a few pre-made formulas on-hand. The vulnerary herbs are used after the infection has passed to help the skin regenerate.
Combinations for Staph Infections
Example 1
- Japanese barberry root 3 pt
- Myrrh reson 3 pt
- Witch hazel inner bark 2 pt
- Licorice root 1
Example 2
- Chaparral leaf 3 pt
- Propolis resin 2 pt
- White oak inner bark 2 pt
- Willow inner bark 1 pt
Herbs that can be applied topically.
Antibacterial
- Chaparral leaf-Larrea tridentata
- Echinacea root-Echinacea purpurea
- Japanese barberry root- Berberis thunbergii
- Myrrh resin-Commiphora species
- Oregon graperoot root-Berberis species
- Pine resin-Pinus species
- Propolis resin-Bee resin
- Yarrow leaf and flower-Achillea millefolium
Antiinflammatory
- Black birch inner bark-Betula lenta
- Licorice root-Glycyrrhiza glabra/G. uralensis
- Willow inner bark-Salix species
- Yarrow leaf and flower-Achillea millefolium
Astringent
- Blackberry root-Rubus species
- White oak inner bark-Quercus alba
- Witch hazel inner bark-Hamamelis virginiana
Vulnerary
- Calendula inflorescence-Calendula officinalis
- Chickweed herb-Stellaria media
- Comfrey root-Symphytum species

Internal Herbal Medicines
Along with external preparation, it is helpful to administer internal herbal medicines for their antibacterial and immune-stimulating properties. These are generally given in tincture form, though it is valuable to have a few available as a glycerite. Along with antibacterial and immune properties, herbal medicines for pain and/or sleep are useful if the infection is causing discomfort. These are given separately from the above categories.
If the infection is healing slowly, it may be beneficial to change the dosage, the combination of herbs, or both.
Before administering a tincture, remember to ask every individual if alcohol is acceptable to them. If it is not, switch to a non-alcohol preparation.
The initial loading dose is often about 4 ml, which is diluted in a 3 oz cup of water (usually followed by a water chaser due to the flavor). The patient can be given a labeled to-go bottle to take the preparation throughout the day without coming back to the first aid station.
The plastic bottles I use have caps rather than droppers (cost savings), and their dosage instructions are by the capful rather than the dropperful. The current bottle caps are 3 ml when filled. The dosage is usually about 1 capful 3 times daily. This comes out to about 2 ml per dosage as we dilute the medicine by about 1/3 so that it is easier to take. This will empty the thirty ml bottle in 3 1/3 days (3 ml x 3 times daily), and it may be refilled once or twice during the course of an event.
Each hand-written label should at least have the dosage. It can be helpful to have the practitioner’s name on the label so the patient can ask for them if they come back. It could also have the herbs and approximate parts so the formula can be replicated.
The pain and sleep remedies are taken as needed.
Combinations-Internal Preparations
Example 1
- Oregon graperoot root 3 pt
- Echinacea root 3 pt
- Black birch inner bark 1 pt
Example 2
- Echinacea root 3 pt
- Myrrh resin 3 pt
- Yarrow leaf and flower 2 pt
- Licorice root 1 pt

Herbs for internal use
Herbs for internal use
Antibacterial
- Chaparral leaf-Larrea tridentata
- Echinacea root-Echinacea purpurea
- Japanese barberry root-Berberis thunbergii
- Myrrh root-Commiphora species
- Oregon graperoot root-Berberis species
- Pine resin-Pinus species
- Propolis resin-Bee resin
- Yarrow leaf and flower-Achillea millefolium
Antiinflammatory
- Black birch inner bark-Betula lenta
- Licorice root-Glycyrrhiza glabra/G. uralensis
- Willow inner bark-Salix species
- Yarrow-leaf and flower-Achillea millefolium
Pain and Sleep Herbs
- California poppy whole plant-Eschscholtzia californica
- Hops strobile-Humulus lupulus
- Jamaican dogwood inner bark-Piscidia piscupula
- Skullcap whole herb-Scutellaria lateriflora
- Valerian root-Valeriana officinalis
- Wild lettuce processed-Lactuca species

Wrapping the Wound
Avoid using sticky tapes to hold dressings in place for staph infections. This is important as the staph bacteria can infiltrate cuts and small openings. When the tape is removed, it will also detach hairs leaving an area for the staph to colonize.
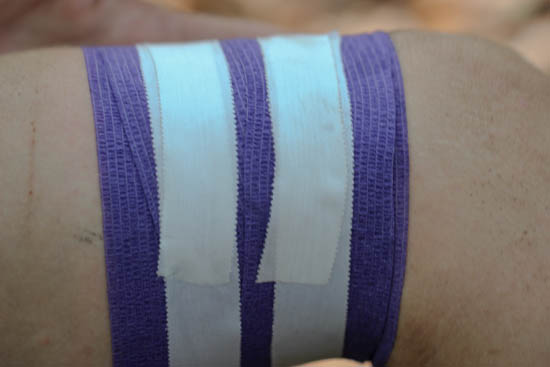
The activated charcoal poultice or herbal gauze pads can be held in place with a cohesive conforming bandage (Coban, Vetrap, and other trade names). These bandages adhere to themselves but not to skin or hair, making them easy to apply and remove. They are not reused but discarded after each use. Tape can be used to hold these bandages in place, but apply the tape to the outside of the cohesive bandage, not to the skin.
If the infection is in a place where you cannot wrap a bandage around it, such as the buttocks, use conformable cloth tape (such as Medipore) to hold the gauze in place.
These bandages should be snug enough to keep the gauze in place but not too tight to impair movement or circulation.
End Notes
While herbal medicine has an important place in first aid, including treating staphylococcus aureus infections, it is crucial for the herbalist to understand the depth of their clinical and assessment skills and when they need to seek further assistance. This might be for diagnosis, treatment, or both. It is also important to know which modality of medicine or treatment will work best for an individual patient and their condition, whether it is herbal, conventional, or other.
For herbalists looking to gain these skills, they may inquire at health care teams at events and ask how they might fit in. If they are new to treating in these situations, they will be in an observational role. They can offer to help out by maintaining the premises or other jobs that need to be done.
As you can see from this article, treating staphylococcus aureus infections requires more than just knowledge about what herbs might be effective. It is essential to understand how to evaluate the infection, maintain sanitary conditions, to educate and give the patient agency to make their own informed decisions, and knowing what treatments might be most applicable and available. With this knowledge, herbalists can lend a helpful hand in treating these prevalent infections.
